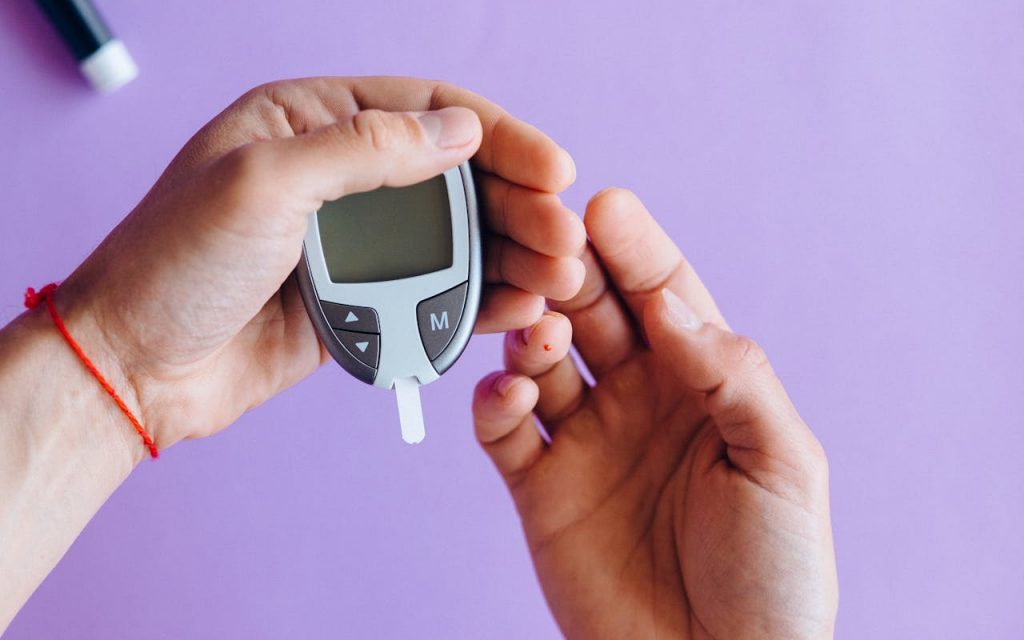
What are Diabetic Ulcers?
Dealing with diabetic ulcers can be a challenging and often overwhelming experience for individuals managing diabetes. These ulcers, which typically occur as breaks or holes in the skin that are slow to heal, can lead to significant health concerns if not managed with vigilant care and attention. If you, or someone you care about, is living with diabetes, here’s what you need to know about diabetic ulcers, their causes, symptoms, and available treatments.
Diabetic ulcers are wounds that typically occur on the feet or lower legs of individuals with diabetes. These ulcers can range from superficial wounds involving only the skin to deeper wounds that extend down to the bone. Due to compromised circulation and nerve damage (peripheral neuropathy), individuals with diabetes may not feel pain or notice injuries to their feet, allowing ulcers to develop and worsen if not properly managed.
Risk Factors
Several factors increase the risk of developing diabetic ulcers, including:
- Peripheral Neuropathy: Reduced foot sensation makes it difficult to detect injuries or irritation.
- Peripheral Vascular Disease: Poor blood flow to the feet hinders the healing process.
- Foot Deformities: High-pressure areas caused by foot deformities can lead to ulcer formation.
- Poor Footwear: Ill-fitting shoes or improper foot hygiene contribute to increased risk.
Diabetic Ulcer Signs and Symptoms
Recognizing the signs and symptoms of diabetic ulcers is crucial for early intervention. Common symptoms include:
- Redness and Heat: The affected area may appear red and feel warmer than the surrounding skin.
- Pain or Sensation: Depending on nerve damage, individuals may experience burning, itching, or pain.
- Drainage: Fluid or blood may be visible on socks or inside shoes.
- Visible Breaks in the Skin: Calluses, cracks, or open wounds may be observed.
- Odour: Foul-smelling discharge from the ulcer is common.
Causes
Diabetic ulcers can develop due to various reasons, including:
- Foot Deformities: Misshapen feet can create pressure points that lead to ulceration.
- Trauma: Injuries such as stepping on sharp objects or wearing inappropriate footwear.
- Poor Circulation: Reduced blood flow slows down the healing process.
- Foot Hygiene: Neglecting foot care practices increases susceptibility to infections.
Treatment Options
Effective treatment of diabetic ulcers involves a multidisciplinary approach and may include:
- Debridement: Removal of dead or infected tissue to promote healing.
- Specialized Dressings: Using ointments and dressings that facilitate wound healing.
- Pressure Relief: Devices like diabetic walking boots are designed to offload pressure from the ulcerated area.
How PBO Group Can Help
When it’s determined that an individual with diabetic ulcers could benefit from a wound care device, the patient’s doctor can refer them to PBO Group to have a custom device made. These devices include:
- Removable Diabetic Walking Boot: This device features a rocker sole and custom insole to reduce pressure on ulcers located on the bottom of the foot.
- Non-Removable Diabetic Walking Boot: This device is similar to the removable boot but is equipped with features to prevent removal. It is often used to support patients with cognitive impairments or non-compliance issues.
- Custom Made CROW Boot: CROW stands for Charcot Restraint Orthotic Walker. This device is designed to provide total contact over the foot, shin, calf, and ankle, effectively reducing pressure on ulcers in various areas.
Another important way PBO Group helps clients living with diabetic ulcers is by helping them research and apply for funding programs that assist with the costs of these devices. Some new programs are being introduced in certain regions of Ontario, with the Ministry of Health covering device costs if the device is prescribed by a physician. Be sure to ask your PBO Group Clinician about funding availability in your region.
Next Steps
Managing diabetic ulcers requires proactive care, proper medical attention, and access to specialized wound care devices. When left untreated, diabetic ulcers can result in the need to surgically amputate the infected toe, part of the foot, and, in some cases, even the whole foot or lower leg. By understanding the causes, symptoms, and treatment options available, individuals with diabetes can take proactive steps to prevent complications and promote healing. If you or someone you know is living with diabetes and experiencing foot-related issues, seeking prompt medical advice can make a life-changing difference. Your PBO Group Clinician is available to support you. Book an appointment here.